
11
Mar
The Science Behind Ketamine-Assisted Therapy

Ketamine-assisted therapy (KAT) is gaining traction as a potential solution for treatment-resistant mental health conditions. KAT combines low-dose ketamine administration with psychotherapy sessions, aiming to create an open mind-state that facilitates deeper exploration and emotional processing alongside a therapist. While ketamine is not a new medication, its use with therapy has shown promise for those who haven’t found relief with traditional treatment methods for mood disorders.
This guide by Caledon Clinic will explore the science behind KAT in Canada, exploring the history of ketamine and how ketamine is used, and ultimately, helping you determine if KAT might be a suitable option for your mental health journey.
Understanding Ketamine
History of Ketamine
Many new and improved treatment options have been discovered in medicine in the last 100 years due to countless scientific breakthroughs. Until recently, ketamine was exclusively used as an anesthetic; however, in recent years, medical and psychological researchers have consistently found that ketamine can be used in many mental health conditions as well.
Discovery and Medical Uses of Ketamine
1950’s Anesthesia PCP
In the 1950s, doctors and chemists were exploring new ways to manage pain during surgery, leading to the discovery of PCP (phencyclidine) by Parke-Davis and Company’s laboratories in Detroit, Michigan, USA.
1960’s Creation of Ketamine
In 1962, ketamine was first synthesized by scientist Calvin Stevens at Parke-Davis. Ketamine emerged as an alternative to PCP. Initially tested on volunteer prisoners, ketamine was found to have similar anesthetic and analgesic properties but with less negative side effects. Following this initial research, ketamine was characterized as a dissociative anesthetic.
1970’s French Clinical Trials
During the 1970s, clinical trials in France further explored the potential of ketamine. While it was considered less potent than PCP, ketamine was recognized for its potent analgesic effects. However, its hallucinogenic side effects were seen as a drawback at the time. Despite this, the U.S. Food and Drug Administration approved ketamine for use as a field anesthetic during the Vietnam War.
Recreational Use of Ketamine
Due to its dissociative and psychedelic effects, ketamine also gained popularity as a recreational drug. In the 1980s, ketamine started to be used in underground rave scenes and eventually made its way into mainstream club culture. Its ability to produce euphoria, hallucinations, and out-of-body experiences attracted individuals seeking a unique high.
From 1978 onward, ketamine became a Class III substance under the US Controlled Substances Act in 1999. This means that Health Canada has approved ketamine for medical use, particularly for treatment-resistant depression, under strict conditions to make sure patients stay safe. However, ketamine remains a controlled substance under the Controlled Drugs and Substances Act. This classification regulates its use and distribution to prevent misuse and address concerns related to its recreational abuse.
Current Research on Ketamine
In recent years, research has shown that ketamine holds promise in treating a range of mental health conditions, including treatment-resistant depression, anxiety, PTSD, and chronic pain. Now, Ketamine is widely used in medical settings; ketamine injections and nasal spray continue to aid a variety of issues in productive ways. Ongoing research continues to explore ketamine’s potential for treating various mental health conditions.
Chemical Properties of Ketamine
Ketamine’s chemical properties play a vital role in its therapeutic effects. Let’s explore its structure and how it interacts with the brain.
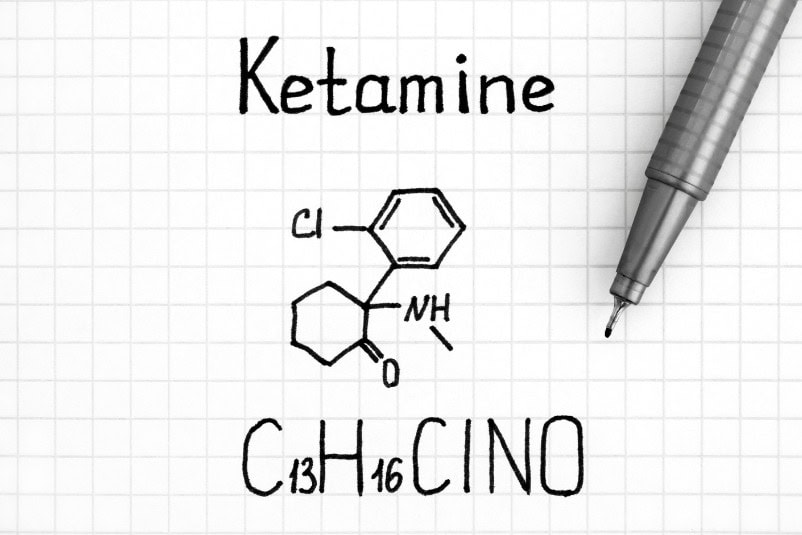
Chemical Structure
The chemical name for ketamine is 2-(2-chlorophenyl)- 2-(methylamino)-cyclohexanone (C13H16ClNO). There are two mirror-image forms of ketamine, which exhibit differing degrees of affinity for their targets. The most common pharmaceutical formulations contain half of either form.
Interactions with Brain Receptors
Ketamine’s therapeutic effects come from its interaction with specific receptors in the brain. During treatment, ketamine primarily targets the N-methyl-D-aspartate (NMDA) receptor, an important player in brain communication. By blocking these receptors, it disrupts the flow of information between neurons, resulting in mood-altering and dissociative effects.
Ketamine is also known to interact with other receptor systems, which is why it can have so many different effects on people. Researchers are still learning how ketamine impacts the brain, but this ongoing exploration is necessary to understand its potential for treating mental health conditions.
Mechanisms of Action in the Brain
Ketamine’s pain-relieving effects stem from its complex interactions within the brain. By modifying neurotransmitter activity and blocking specific pain pathways, ketamine can provide rapid and effective relief. Here’s a closer look:
NMDA Receptor Antagonism
A key mechanism involves its action on N-methyl-D-aspartate (NMDA) receptors. These receptors play a crucial role in pain signal transmission and central sensitization, where pain pathways become hypersensitive. Ketamine acts as an NMDA receptor antagonist, essentially blocking the stimulation of these pathways and reducing the perception of pain.
Glutamate System
Glutamate is the brain’s primary excitatory neurotransmitter, making it a large contributor to signaling pain. Ketamine interacts with the glutamate system in various ways, potentially modulating its activity and contributing to its analgesic effects. By blocking NMDA receptors, ketamine reduces the excitatory actions of glutamate, which can lead to a decrease in the perception of pain and an overall calming effect on the nervous system.
Synaptic Plasticity
Chronic pain and depression can lead to changes in how brain cells communicate (synaptic plasticity). Ketamine may help reset this plasticity, promoting a return to normal neural processing and reducing chronic symptoms. By influencing synaptic connections and strengthening neural pathways, ketamine can potentially reverse maladaptive changes caused by chronic pain and depression, thereby improving overall brain function and patient well-being.
Ketamine in Medical Use
Anesthesia
Ketamine is a licensed anesthetic in Canada. However, for off-label use in treating mental health conditions, each province has its own set of regulations.
At anesthetic doses, ketamine induces a trance-like state providing pain relief, sedation and amnesia. There are several characteristics that distinguish this type of anesthesia, including preserved breathing and airway reflexes, increased heart rate and blood pressure, and moderate bronchodilation.
Early Uses in Surgery
During the Vietnam War, ketamine became a mainstay in battlefield medicine due to its effectiveness in treating wounded soldiers without the need for complex respiratory support. Its unique properties also proved advantageous in pediatric settings, where maintaining airway control can be challenging.
In the 1970s, ketamine gained wider acceptance, mainly for procedures that need minimal muscle relaxation, like pain management during dressing changes or minor surgeries. In the 1980s, research explored the potential for ketamine to manage chronic pain. The focus shifted in the 1990s to be used with other anesthetics, offering more pain relief benefits.
Dosage and administration
Ketamine is both water and lipid soluble, meaning it can be administered in many ways, including intramuscularly, intravenously, nasally, orally, and subcutaneously. The appropriate dosage depends on the intended use and the patient. In surgery, ketamine is typically used with other medications for optimal pain control with minimal side effects.
Pain Management
While traditionally used as an anesthetic, ketamine is now being explored for chronic pain conditions that haven’t responded well to other treatments, especially those that have a neuropathic component.
Currently, some clinics offer low-dose ketamine infusions under specialist supervision for chronic pain conditions like complex regional pain syndrome (CRPS), post-herpetic neuralgia, fibromyalgia, and more. These treatments aim to target pain pathways and offer relief where conventional therapies have failed.
It’s important to note that ketamine is not a first-line treatment and should be discussed with a doctor to determine if it’s a suitable option for your specific situation and location. Factors such as your overall health, medical history, and the severity of your pain condition will play a crucial role in this decision. Additionally, it’s essential to receive treatment from a qualified healthcare provider like Caledon Clinic to ensure the safe and effective use of ketamine.
Ketamine-Assisted Therapy for Mental Health

Ketamine has been used as an addition to psychotherapy since the 1970s and is becoming more widely accepted as a safe and effective tool to add to therapy for several mental health conditions. This section will explore ketamine-assisted therapy (KAT) and its growing role in treating treatment-resistant conditions.
It’s important to note that ketamine-assisted therapy (KAT) is only recently approved for use in Canada, and research is continuing solidify its place in standard treatment protocols. However, current results are promising, offering hope for individuals struggling with treatment-resistant mental health conditions.
Depression and Ketamine
Research suggests that ketamine can produce rapid and significant reductions in symptoms of depression, usually in hours of administration. This contrasts with traditional antidepressants, which can take weeks or even months to show their full effects. Such a swift response can be particularly beneficial for individuals experiencing severe depressive episodes or those who have not found relief with conventional treatments.
Some studies compare ketamine to traditional antidepressants and highlight key differences. Ketamine works through a different mechanism, targeting neuroplasticity rather than altering brain chemistry. This means that ketamine enhances the brain’s ability to form new connections and pathways, which may explain its faster-acting effects. Traditional antidepressants, on the other hand, typically focus on altering the levels of neurotransmitters like serotonin and norepinephrine in the brain, a process that unfolds more slowly.
It’s important to note that ketamine is not a cure for depression, and its long-term benefits are still under investigation. While ketamine therapy offers hope for rapid symptom relief, the effects of ketamine tend to diminish over time, necessitating ongoing treatment. Researchers are actively exploring ways to prolong the benefits of ketamine and integrate it into broader treatment plans.
As research continues, the hope is that ketamine will become a well-established option within the spectrum of depression treatments, offering rapid relief and improving the quality of life for those affected by this condition.
Treatment-Resistant Depression
Treatment-resistant depression (TRD) is a form of depression that doesn’t respond adequately to at least two different types of traditional antidepressants. Research suggests that ketamine can be highly effective in reducing symptoms, even in individuals who haven’t found relief with other treatments.
Studies have shown significant improvements in mood, motivation, and overall well-being following ketamine infusions. While more research is needed, KAT is emerging as a valuable tool for managing TRD.
Other Psychiatric Disorders
While research on KAT primarily focuses on depression, there’s growing interest in its potential for other mental health conditions, like anxiety, PTSD, and bipolar disorder. In addition to these, KAT is being explored for its efficacy in treating obsessive-compulsive disorder (OCD), where traditional treatments often fall short.
Emerging studies suggest that ketamine’s rapid action on neurotransmitter systems may provide relief for patients with chronic suicidal ideation, offering a critical intervention in acute mental health crises. Furthermore, there’s curiosity around its application for substance use disorders, particularly in alleviating cravings and reducing relapse rates.
For these conditions, it’s important to emphasize that KAT is still in the early stages of investigation. More research is needed to determine long-term safety and efficacy for mental health disorders.
Conclusion
Overall, ketamine’s transition from a surgical anesthetic to mental health is a fascinating example of scientific ingenuity.
Key takeaways include the promise of KAT for treatment-resistant depression, its unique mechanism of action that promotes neuroplasticity, and its potential application for other mental health conditions like anxiety and PTSD. However, continued research is crucial to solidify KAT’s place in standard treatment protocols, ensuring long-term safety and efficacy. Ethical considerations regarding patient selection, ketamine administration, and integration with psychotherapy are more important than anything else.
Despite these ongoing investigations, the potential of KAT to offer relief to those struggling with treatment-resistant mental health challenges is a significant development. As research continues, ketamine-assisted therapy has the potential to revolutionize the landscape of mental healthcare.
Here at Caledon Clinic, our team of specialists is committed to providing ketamine medication combined with psychotherapy to provide evidence-based, safe, compassionate care to promote healing that lasts.
Contact Caledon Clinic today to learn more about how KAT may help you reclaim your mental well-being.


